Genetics and Depression: Can Your Genes Really Cause Depression?
Mental Health
Can genetics cause depression?
Genetics can increase a person’s risk of developing depression, but they do not directly cause the condition on their own. Research suggests that depression is influenced by a combination of genetic factors, brain chemistry, and environmental experiences such as stress or trauma. People with a family history of depression may have a higher vulnerability, but lifestyle, support systems, and treatment can significantly reduce the risk.
Introduction
Depression is one of the most common mental health conditions worldwide, affecting millions of individuals every year. In recent decades, researchers have increasingly focused on understanding the biological and genetic foundations of mental health disorders. Among the most frequently asked questions in mental health science is whether depression can be inherited through genetics.
Many individuals who have family members struggling with depression worry about whether they might eventually develop the same condition. While emotional stress, trauma, and lifestyle factors clearly contribute to depression, scientific evidence shows that genetic factors also play a significant role in shaping a person’s vulnerability to the disorder.
However, the relationship between genetics and depression is complex. Depression is not caused by a single gene, nor does having a family history guarantee that someone will develop the disorder. Instead, researchers describe depression as a multifactorial condition, meaning it develops through a combination of genetic susceptibility and environmental triggers.
Understanding the connection between genetics and depression is essential for improving prevention, early detection, and treatment strategies. By identifying how genetic variations affect brain chemistry, stress response, and emotional regulation, scientists hope to develop more personalized approaches to mental health care.
In this comprehensive guide, we will explore how genes influence depression risk, how family history affects mental health, and what individuals can do to reduce their vulnerability even when genetic factors are present.
What Is Depression?
Depression is a mood disorder characterized by persistent feelings of sadness, hopelessness, and loss of interest in activities that were once enjoyable. Unlike temporary emotional distress, clinical depression can last for weeks or months and may significantly interfere with daily life.
Depression affects how a person thinks, feels, and behaves. It may influence energy levels, sleep patterns, appetite, concentration, and emotional responses. In severe cases, depression can lead to difficulties maintaining relationships, working productively, or caring for oneself.
Common symptoms of depression include:
- Persistent sadness or low mood
- Loss of interest in hobbies or activities
- Fatigue and lack of motivation
- Changes in appetite or weight
- Sleep disturbances
- Difficulty concentrating
- Feelings of worthlessness or guilt
- Thoughts of death or suicide
While these symptoms can vary from person to person, researchers believe that both biological factors and environmental experiences contribute to their development.
Is Depression Genetic?
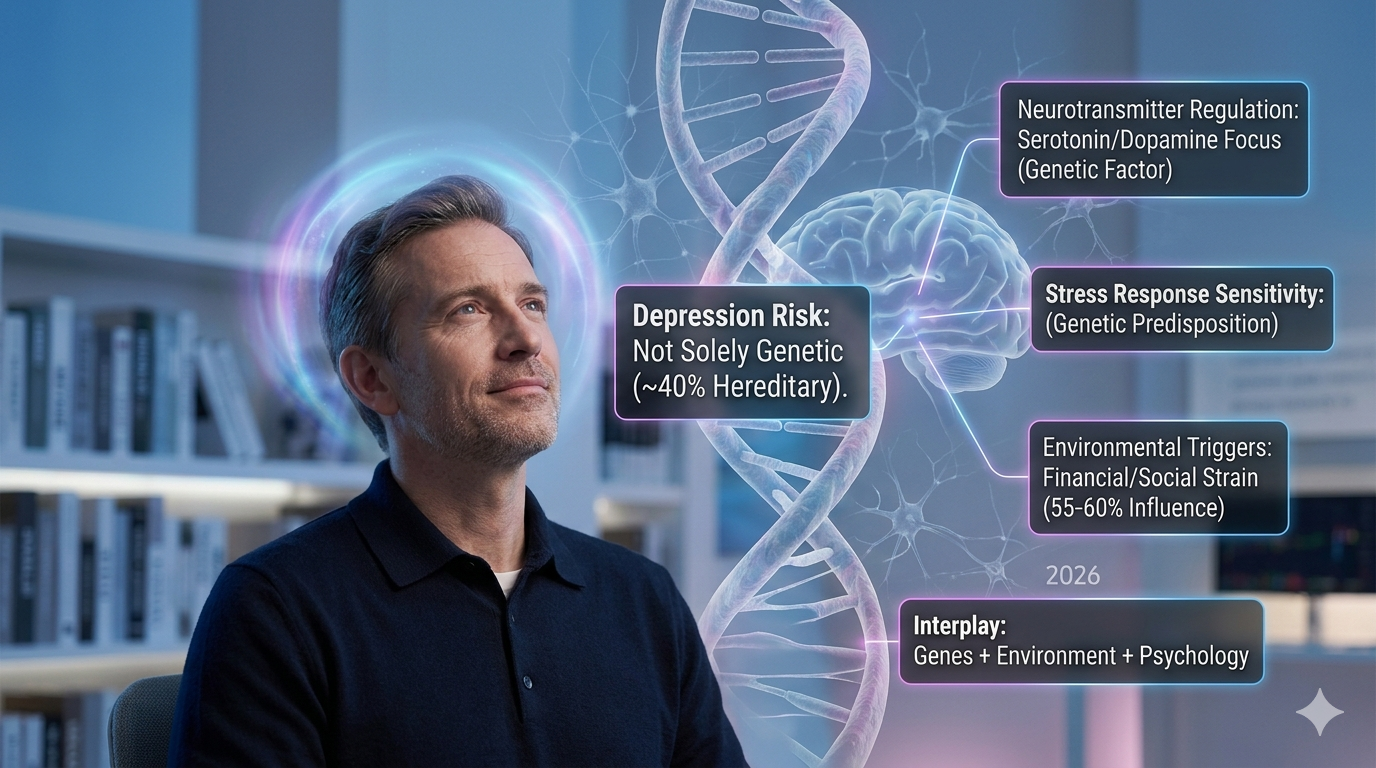
One of the most important questions in mental health research is whether depression can be inherited. Studies suggest that genetics may account for approximately 30% to 40% of a person’s risk of developing depression.
This means that individuals with a family history of depression are statistically more likely to experience depressive symptoms during their lifetime. However, genetics alone do not determine whether someone will develop the disorder.
Instead, genes influence biological processes such as:
- Brain chemistry
- Stress response systems
- Emotional regulation
- Neurotransmitter activity
When these biological vulnerabilities interact with life stressors, the risk of depression increases. This concept is known as gene–environment interaction, a central theory in modern mental health research.
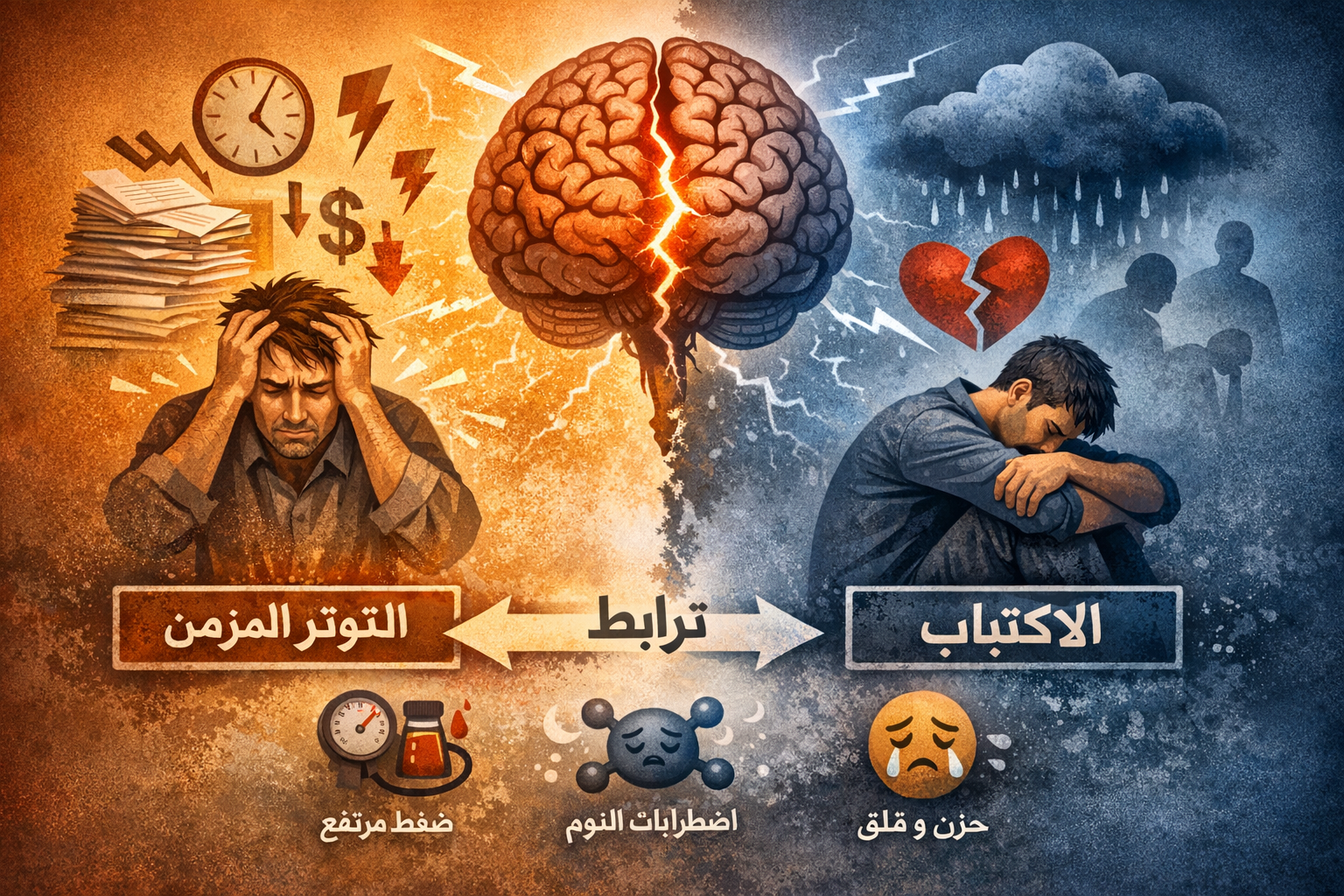
How Genes Influence Brain Chemistry
Genes contain instructions that determine how the body produces proteins, enzymes, and neurotransmitters. These biological elements are essential for normal brain function and emotional stability.
Several neurotransmitters play a key role in mood regulation:
Serotonin
Serotonin is often referred to as the “feel-good” neurotransmitter. It helps regulate mood, sleep, and appetite. Low serotonin activity has been associated with depression.
Dopamine
Dopamine is involved in motivation, reward, and pleasure. Reduced dopamine activity may contribute to feelings of apathy and lack of motivation.
Norepinephrine
Norepinephrine influences alertness, energy, and stress response. Imbalances in this neurotransmitter can contribute to depressive symptoms.
Genetic variations affecting these neurotransmitter systems may increase vulnerability to depression, especially when combined with stressful life experiences.
The Role of the Serotonin Transporter Gene
One of the most studied genetic variations associated with depression involves the serotonin transporter gene, often referred to as 5-HTTLPR.
This gene affects how serotonin is transported between brain cells. Certain variations of this gene may increase emotional sensitivity to stress, which can raise the likelihood of developing depression following difficult life events.
However, possessing this gene variant does not guarantee depression. Many people with this genetic profile never develop mental health disorders, highlighting the importance of environmental and psychological factors.
Family History and Depression Risk
Family history is one of the strongest indicators of potential depression risk. Studies involving twins and families provide valuable insights into how genetics contribute to mental health.
Research findings suggest:
- Individuals with one depressed parent have an increased risk of depression
- Having two parents with depression significantly increases vulnerability
- Identical twins show higher similarity in depression risk compared to fraternal twins
Despite these patterns, genetics do not determine destiny. Many individuals with strong family histories of depression remain mentally healthy due to protective environmental factors.
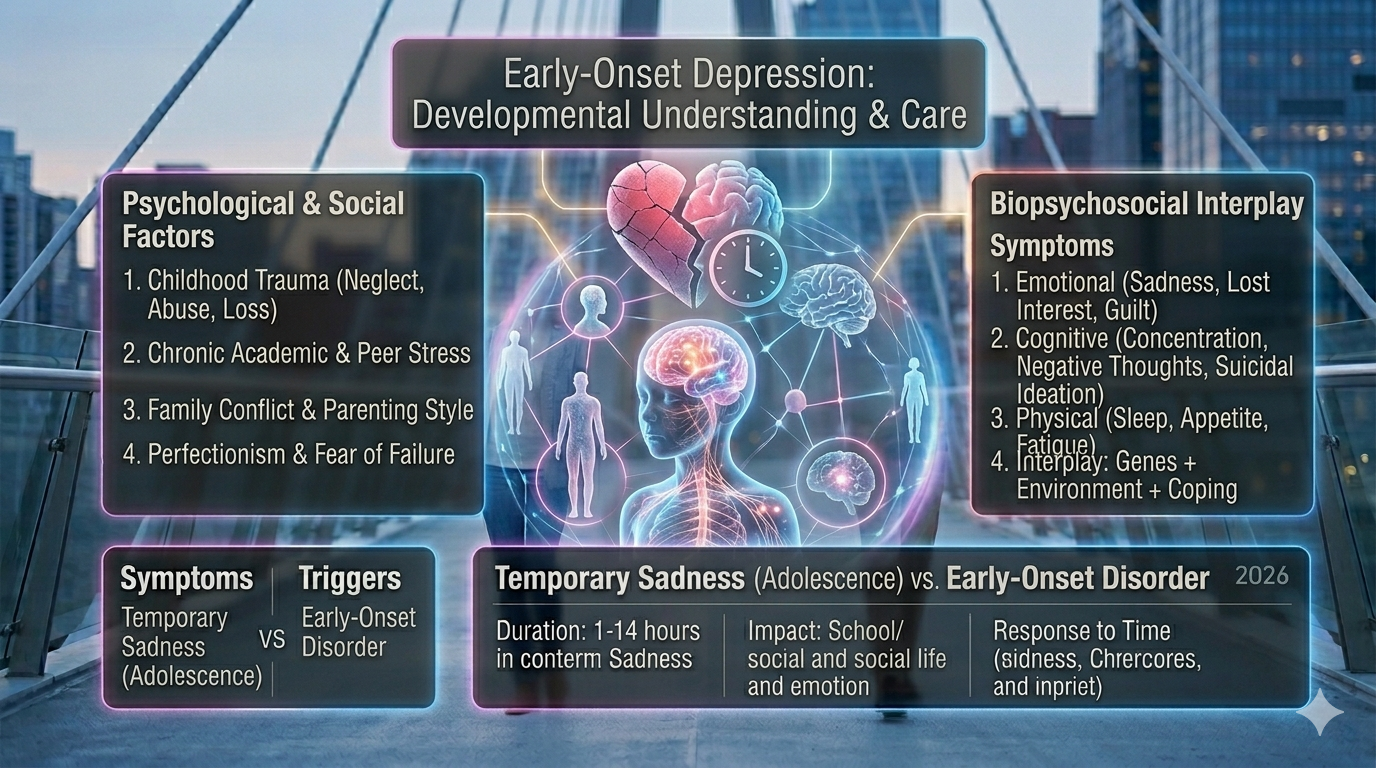
Environmental Triggers That Interact With Genetic Risk
Even when genetic vulnerability exists, depression often requires environmental triggers to develop. These triggers can include a wide range of life experiences.
Common environmental factors associated with depression include:
- Chronic stress
- Childhood trauma
- Relationship conflicts
- Financial hardship
- Loss of loved ones
- Social isolation
- Major life transitions
The interaction between genetic susceptibility and environmental stressors explains why some individuals develop depression while others with similar genetics do not.
Epigenetics and Depression
In recent years, scientists have begun exploring the role of epigenetics in mental health. Epigenetics refers to changes in gene expression that occur without altering the DNA sequence itself. Environmental experiences such as stress, trauma, nutrition, and lifestyle can influence how genes are activated or deactivated.
For example, prolonged stress may modify gene activity related to stress hormones, potentially increasing vulnerability to depression. This discovery suggests that environmental conditions can shape how genetic risk factors influence mental health outcomes.
Can Genetic Testing Predict Depression?
Genetic testing for mental health risk is still in the early stages of development. While certain tests analyze genes involved in neurotransmitter regulation, they cannot accurately predict whether someone will develop depression.
However, genetic testing may still offer useful insights for medical professionals. Potential benefits include:
- Understanding medication response
- Reducing trial-and-error prescribing
- Identifying biological risk patterns
As research advances, personalized mental health care based on genetic information may become more common.
Prevention Strategies for People With Genetic Risk
Even when depression runs in a family, many preventive strategies can reduce the likelihood of developing the condition. Healthy lifestyle habits are among the most effective protective factors.
Key prevention strategies include:
- Regular physical activity
- Balanced nutrition
- Healthy sleep routines
- Stress management techniques
- Strong social support networks
- Professional counseling when needed
Exercise, in particular, has been shown to increase serotonin and dopamine levels, which may counteract biological vulnerabilities.
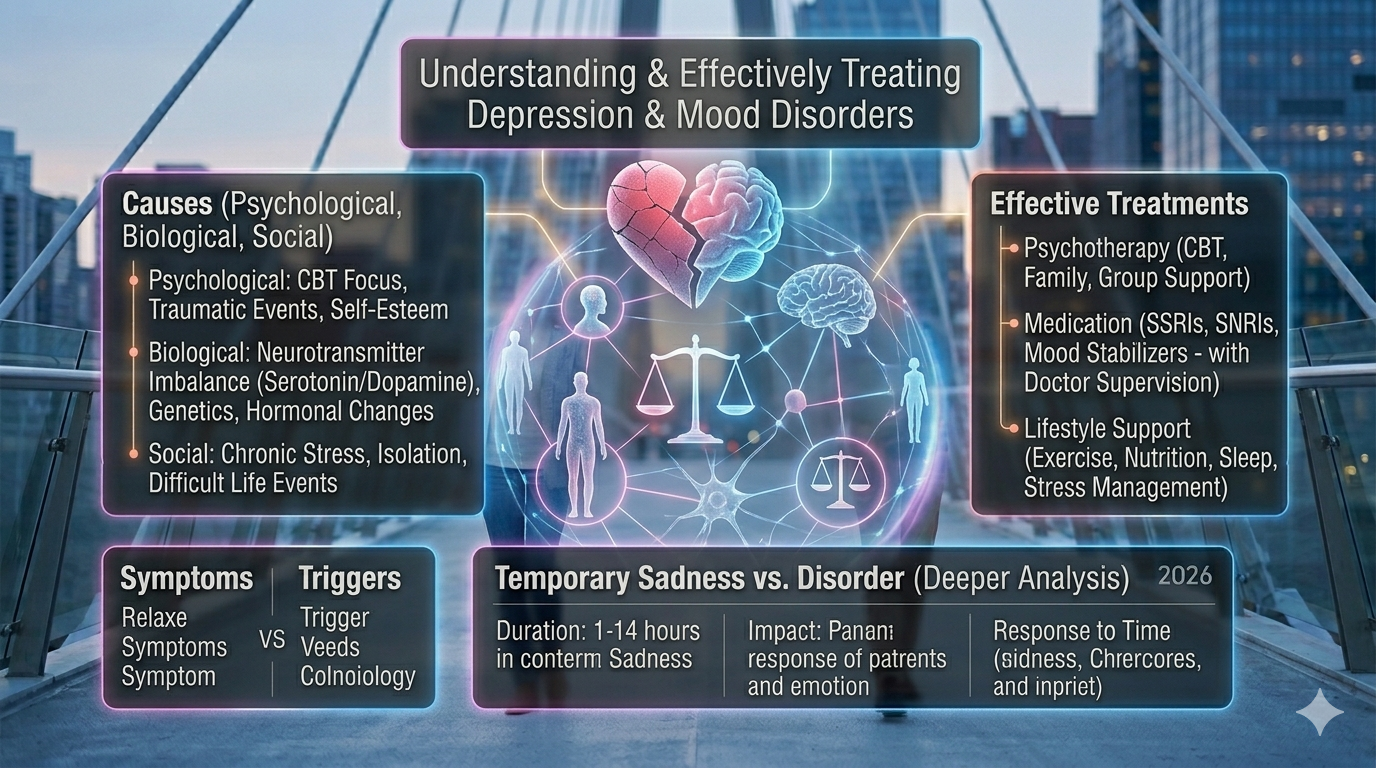
Effective Treatments for Depression
If depression develops, numerous effective treatments are available. Modern mental health care often combines multiple approaches to achieve the best outcomes.
Psychotherapy
Psychological therapy helps individuals understand negative thought patterns and develop healthier coping strategies. Cognitive Behavioral Therapy (CBT) is one of the most widely used treatments for depression.
Medication
Antidepressant medications help regulate neurotransmitter activity in the brain. These medications can be especially beneficial when depression has a strong biological component.
Lifestyle Changes
Regular exercise, improved sleep habits, and balanced nutrition can significantly enhance recovery.
Combined Treatment
Research consistently shows that combining therapy and medication often produces the most effective results for moderate to severe depression.
People Also Ask
Is depression hereditary?
Depression can have a genetic component. Individuals with a family history of depression may have a higher risk, but environmental factors and lifestyle also play an important role.
What percentage of depression is genetic?
Studies estimate that genetics contribute about 30% to 40% of the overall risk for depression.
Can depression skip generations?
Yes. Genetic predisposition can appear in some family members while skipping others due to complex gene interactions.
Can lifestyle overcome genetic depression risk?
Healthy lifestyle habits, stress management, therapy, and supportive relationships can significantly reduce depression risk even in individuals with genetic vulnerability.
FAQ
Can depression be inherited from parents?
Yes, depression can run in families due to shared genetic factors, but inheritance does not guarantee that someone will develop the condition.
Are genetic forms of depression harder to treat?
Not necessarily. Many individuals with genetic vulnerability respond well to therapy, medication, and lifestyle changes.
Do antidepressants work differently for genetic depression?
In some cases, genetic differences can influence how individuals respond to medications. This is why doctors sometimes use pharmacogenetic testing.
Can early intervention reduce genetic depression risk?
Yes. Early awareness, stress management, and psychological support can significantly reduce the impact of genetic predisposition.